Conventional vs. Reverse Total Shoulder Replacement
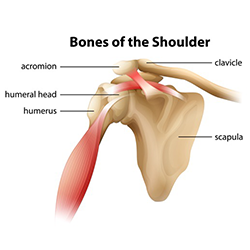
Although shoulder joint replacement is less common than knee or hip replacement, it is successful in relieving shoulder joint pain and improving arm mobility. About 53,000 people in the U.S. have shoulder replacement surgery each year, according to the Agency for Healthcare Research and Quality. The shoulder is made up of three bones: upper arm bone (humerus), shoulder blade (scapula), and the collarbone (clavicle). The head of the upper arm bone fits into a rounded socket (glenoid). The shoulder is a ball-and-socket joint. The surfaces of the bones where they touch are covered with articular cartilage, which protects the bones and enables them to move easily. A thin tissue, synovial membrane, covers all remaining surfaces inside the shoulder joint. A combination of muscles and tendons, the rotator cuff, keeps the arm bone centered in the shoulder socket, providing stability, support and enabling the shoulder to rotate through a greater range of motion than any other joint in the body.
In a conventional shoulder replacement, the damaged parts of the shoulder are removed and replaced with artificial components, prosthesis. A plastic cup is fitted into the shoulder socket and a metal ball is attached to the top of the upper arm bone. The prosthesis mimics the normal anatomy of the shoulder, using the rotator cuff muscles to function properly. In a reverse total shoulder replacement, the socket and metal ball are switched. The metal ball is fixed to the socket and the plastic cup is fixed to the top of the upper arm bone. For patients with large rotator cuff tears or shoulder arthritis, arthropathy, reverse total shoulder replacement is a better option because the rotator cuff muscles no longer function. The reverse total shoulder replacement relies on the deltoid muscle, instead of the rotator cuff, to position and power the arm.
The DOC orthopedic surgeon will evaluate each shoulder condition and discuss nonsurgical and surgical options with the patient guest. If total or reverse total shoulder replacement is necessary, the surgeon will remove the damaged bone and position the new components to restore shoulder function. The procedure to replace the shoulder joint with prosthesis takes about two hours. After surgery, the patient wears a sling and has limited arm use. DOC physical therapy is recommended to strengthen the shoulder and improve flexibility. Follow-up visits with the DOC surgeon are important in order to monitor shoulder strength, motion, and functionality during the healing and rehabilitation process. Thousands of patients have experienced an improved quality of life after shoulder joint replacement surgery. According to a multicenter study, shoulder replacement surgery results in good to excellent pain relief, improvement in function and patient satisfaction in 95% of cases.
For more information on the cost of care, click here.




